By
and
Not so long ago most of us had at least some semblance of a waist, and when looking straight down could see our toes. Not so much anymore! In fact, far from just being a matter of appearance, the recent epidemic of obesity is a serious public health concern. The World Health Organization (WHO) estimates that more than a half billion adults worldwide are obese, including increasing numbers in developing countries.
At present about 70 percent of adult Americans are overweight, and about 35 percent are obese. Obesity is usually defined by body mass index (BMI), which is a measure of body weight adjusted for height. Normal BMI is considered to be 18-25; 26-29 is labeled overweight; and 30 or higher is labeled obese.
Much of what we know about diet, lifestyle, and health comes from the Adventist Health Studies (AHS) based out of Loma Linda University, studies that have gained much attention for showing that Adventists are a long-lived and healthy group of people. Adventist Health Study-2 (AHS-2), funded by the National Institutes of Health, at present focuses on the connection between diet and cancer risk. It includes the data of more than 90,000 Adventists from across North America.
Do Adventists, however, also have an advantage with body weight? Looking around your local church congregation, you probably already suspect the answer. The average BMI in AHS-2 was 26.9, so on average Adventists in AHS-2 were overweight. We found that 61.1 percent of AHS-2 Adventist men were overweight or obese and 19.0 percent were obese; whereas 55.0 percent of AHS-2 Adventist women were overweight or obese and 25.4 percent were obese (adjusting to the national percentage of Black Americans). It’s interesting that more women than men are obese (especially Black women), but a considerably higher percentage of men as compared to women are in the overweight category. Another striking contrast is that in AHS-1 (nearly 40 years ago and admittedly only White Californians) the average BMI was more than two units lower at 24.6. So we are better off than the U.S. averages. But many North American Adventists are overweight, and this seems to have increased in recent decades.
Does it matter? Yes, it does. In Adventist Health Studies and many other studies, excess weight correlates with higher risk of heart attack, stroke, high blood pressure, diabetes, arthritis, and several common cancers. Some studies also find a higher risk of dementia in heavier elderly persons. It’s been estimated that in the U.S., only smoking exceeds overweight and obesity as an underlying cause of premature death.
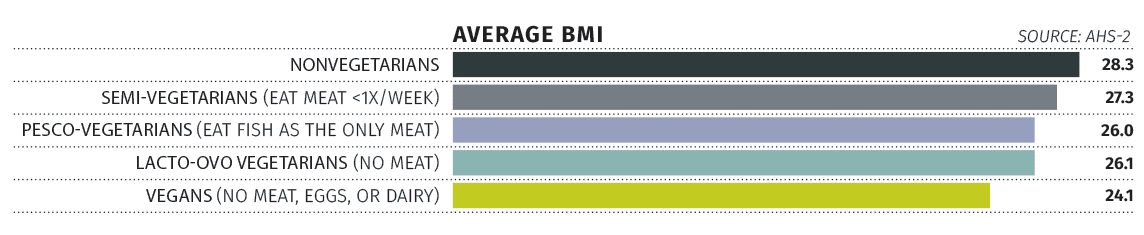
While studying obesity is not the major focus of AHS-1 or AHS-2, they have provided some interesting findings. First, it’s clear from these (and other) studies that on average, vegetarians are less obese than nonvegetarians (see chart). The four-point BMI difference between nonvegetarians and vegans noted in the chart would represent a difference of nearly 30 pounds in persons of average height. Second, BMI in our studies has been linked to a much lower risk of type 2 diabetes and high blood pressure, similar to results from many other studies. Vegetarian Adventists have lower risk of these disorders, probably in part because of their lower BMI.
In AHS-1 five factors were identified that could together predict about 10 years longer life expectancy on average. Not being overweight or obese was one of these. AHS research also indicates that maintaining normal body weight continues to have longevity advantages for seniors, even up to age 90. Together these findings support our understanding that maintaining normal body weight is important for having a long, healthy life, and that vegetarian diets are one approach that helps achieve this.

There are many genetic differences in metabolism and the handling of calories between individuals. Yet differences in genes cannot alone account for our increasing size. This is because the frequency of particular gene variants in a population changes significantly only over many generations, never in just a few decades. The overweight problem must be caused by the environment and lifestyle in the great majority of people. Although very uncommon, untreated medical conditions may also cause weight problems, but for the great majority “bad genes” or “hormonal problems” cannot be the main cause.
Weight loss and maintenance can be huge challenges for people in today’s world. Many of us are surrounded by almost endless opportunities to eat high-calorie weight-promoting foods (even while many others in the world struggle with undernutrition). This is usually coupled with sedentary jobs, high stress, and poor sleep, all of which promote weight gain. Given these challenges, what can we do?
It’s been estimated that in the U.S., only smoking exceeds overweight and obesity as an underlying cause of premature death.
Losing weight is nearly always hard. Some people fight genetic propensities (which do exist), ingrained habits, stressful environments, and emotional overlays. We recognize that structured weight-loss programs and appropriate medical interventions may be necessary to help those with extreme obesity or obesity that is causing or caused by major medical or psychological problems. Here we focus on more common situations in which conceptually simple changes in lifestyle can, with some effort, make a difference.
There are many different opinions about losing weight, and every person and situation is different. Well-publicized “weight-reduction diets” are not necessarily a good approach. Although several of these can result in short-term weight loss, the goal must be a long-term sustainable diet that will not have adverse consequences (such as are suspected for several high-animal-protein diets). We list several simple principles of weight loss on the previous page.
Obesity is clearly a major problem with serious consequences for all of us. But scientific knowledge and sound principles of healthful living can help us make progress. We wish God’s blessing to each of you as you seek to achieve and maintain a normal body weight, and even more important, the best of health.
Gary E. Fraser, M.B.Ch.B., Ph.D., is a professor in the Schools of Public Health and Medicine at Loma Linda University and principal investigator of Adventist Health Studies. Michael J. Orlich, M.D., Ph.D., is assistant professor in the Schools of Medicine and Public Health at LLU and a coinvestigator for AHS.